Angeliki and Karol First Authored Paper Published
Tite: Assessment of antibiotic release and antibacterial efficacy from pendant glutathione hydrogels using ex vivo porcine skin
ABSTRACT:
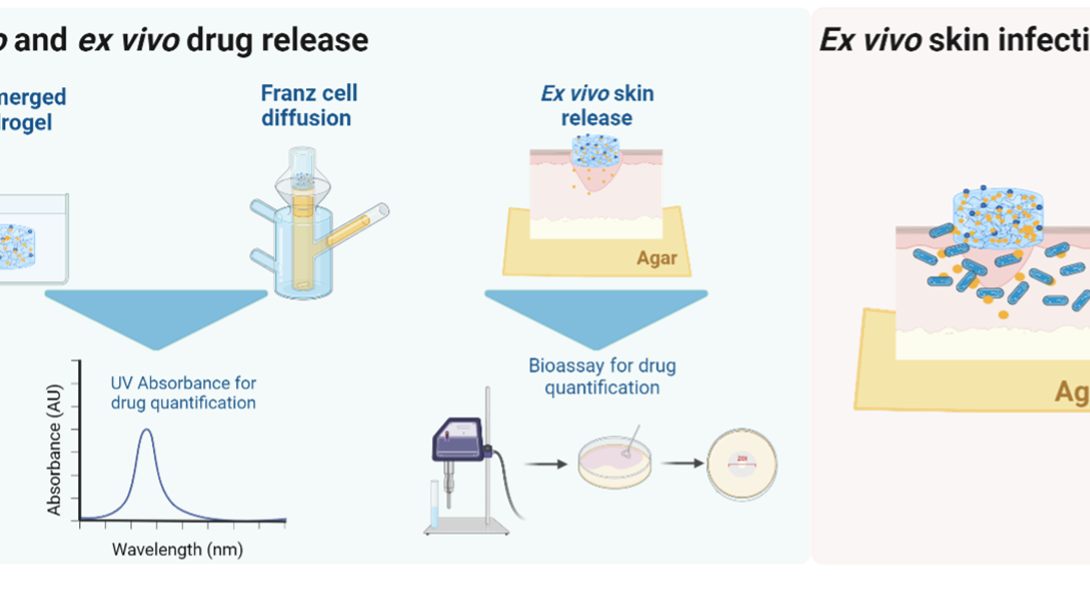
Acute bacterial skin and skin structure infections (ABSSSIs) confer a substantial burden on the healthcare system. Local antibiotic delivery systems can provide controlled drug release directly to the site of infection to maximize efficacy and minimize systemic toxicity. The purpose of this study was to examine the antibacterial activity of antibiotic-loaded glutathione-conjugated PEG hydrogels (GSH-PEG) against ABSSSIs utilizing an ex vivo porcine dermal explant model. Vancomycin- or meropenem-loaded GSH-PEG hydrogels at 3 different dose levels were loaded over 1 hour. Drug release was monitored in vitro under submerged conditions, by the Franz cell diffusion method, and ex vivo utilizing a porcine dermis model. Antibacterial activity was assessed ex vivo on porcine dermis explants inoculated with Staphylococcus aureus or Pseudomonas aeruginosa isolates treated with vancomycin- or meropenem-loaded GSH-PEG hydrogels, respectively. Histological assessment of the explants was conducted to evaluate tissue integrity and viability in the context of the experimental conditions. A dose-dependent release was observed from vancomycin and meropenem hydrogels, with in vitro Franz cell diffusion data closely representing ex vivo vancomycin release, but not high dose meropenem release. High dose vancomycin-loaded hydrogels resulted in a greater than 3 log10 clearance against all S. aureus isolates at 48 hours. High dose meropenem-loaded hydrogels achieved 6.5, 4, and 2 log10 reductions in CFU/ml against susceptible, intermediate, and resistant P. aeruginosa isolates, respectively. Our findings demonstrate the potential application of GSH-PEG hydrogels for flexible, local antibiotic delivery against bacterial skin infections.
KEYWORDS: hydrogel; antibiotic delivery; skin infection; topical drug delivery; ex vivo infection model